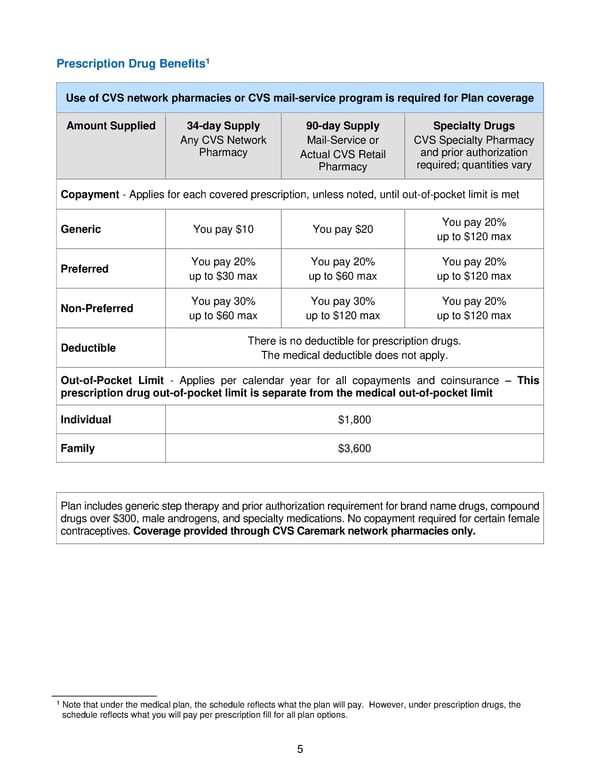
5 Prescription Drug Benefits 1 Use of CVS network pharmacies or CVS mail - service program is required for Plan coverage A mount Supplied 34 - day Supply Any CVS Network Pharmacy 90 - day Supply Mail - Service or Actual CVS Retail Pharmacy Specialty Drugs CVS Specialty P harmacy and pr ior authorization required; quantities vary Copayment - Applies for each covered prescription, unless noted, until out - of - pocket limit is met Generic You pay $10 You pay $20 You pay 20% up to $120 max Preferred You pay 20% up to $30 max You pay 20% up to $60 max You pay 20% up to $120 max Non - Preferred You pay 30% up to $60 max You pay 30% up to $120 max You pay 20% up to $120 max Deductible There is no deductible for prescription drugs. The m edical deductible does not apply. Out - of - Pocket Limit - Applies per calendar year for all copayments and coinsurance – This prescription drug out - of - pocket limit is separate from the medical out - of - pock et limit Individual $1,800 Family $3,600 Plan includes generic step therapy and prior authorization requirement for brand name drugs, compound drugs over $300, male androgens, and specialty medications. No copayment required for certain female contraceptives. Coverage provided through CVS Caremark network pharmacies only. 1 Note that under the medical plan, the schedule reflects what the plan will pay. However, under prescription drugs, the schedule reflects what you will pay per prescription fill for all plan options.
 2018 BTF Plan B Page 9 Page 11
2018 BTF Plan B Page 9 Page 11